Introduction
Plantar fascia is a thick fibrous band from the tubercle of calcaneus (heel bone) towards the toes. [Figure 1] Its function is to support the longitudinal arch of the foot. Plantar fasciitis is inflammation of plantar fascia due to chronic overuse and micro-tears. It affects men and women equally and is most common between the ages of 40 and 60.

Risk Factors
People, who are overweight, have tight Achilles tendon and decreased ankle dorsiflexion or active in playing weight-bearing sports (including dancing and running), are at risk. These sports cause repeated injuries to the plantar fascia from time to time. There are some other predisposing factors including flat feet, inappropriate footwear, running up hills or on sand and etc.
Symptoms
Patients usually present with plantar heel pain which usually increases when standing from sitting or getting up from bed in the morning. At early stage, the pain may ease off after walking. At later stage, the pain may exaggerate after prolong walking or standing during the day.
Signs
There may be tenderness along the sub-calcaneal region and the Achilles tendon might be tight. Flat feet deformity may be associated.
Investigation
It is usually not necessary to have further investigations except when other diagnoses have to be excluded, e.g. stress fracture, tarsal tunnel syndrome etc. In that case, x-ray and magnetic resonance imaging (MRI) will be required.
Treatment
Conservative treatment
1. Rest – Simple measures are important. Try to avoid if there is any trigger of pain, such as sudden increase in pain after high-impact exercise. Try to decrease the amount of physical activities, especially impact sports, to allow your plantar fascia to rest.
2. Ice therapy and anti-inflammatory drugs – During the acute phase, the aim of treatment is to reduce pain and inflammation. Ice therapy could be applied to the affected area for 20 minutes 3 times per day. Non-steroidal anti-inflammatory drugs such as Ibuprofen can be used to reduce pain and swelling.
3. Ultrasound therapy – It can be administered by physical therapist to reduce pain and swelling around the heel. It targets a combination of high frequency low amplitude sound waves to the affected plantar fascia, which may break down the inflamed tissue.
4. Extracorporeal shock wave therapy – Sound waves are used to enhance healing over the heel area for chronic pain not responded to other conservative means.
5. Physio therapy – A physio therapist could help with deep tissue massage and specific stretching exercises to relieve stress to the plantar fascia. Daily stretching of plantar fascia and calf muscles is recommended. [Figure 2]
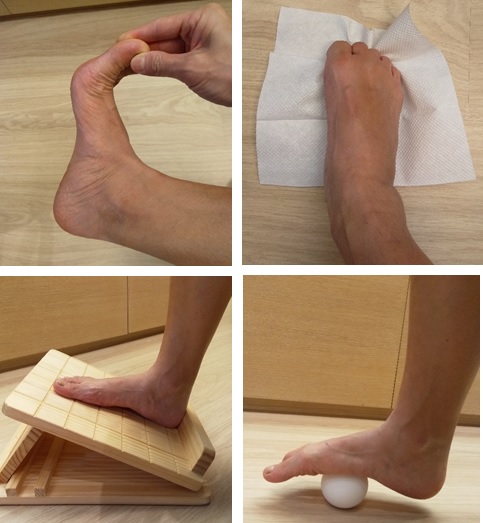
Upper left: Bend your ankle and toes up.
Upper right: Pick up towel and hold it.
Bottom left: Stretch the plantar fascia on any stretch board. Alternatively stand against the wall, place one leg in front of the other, bend your knee and lean forward until you feel the stretch in your calf.
Bottom right: Roll a ball under your foot.
6. Orthosis – Wearing shoes with good arch support can relieve symptoms. Additional insoles can sometimes provide extra support to the foot and distribute the stress more evenly. It is especially important in patients with flat foot deformity.
7. Weight reduction – Overweight is one of the risk factors for developing plantar fasciitis. It increases stress on the plantar fascia. Therefore, weight reduction is recommended.
8. Injections – Injection with steroid or platelet-rich plasma (PRP) could be considered for persistent pain after the above measures. Multiple injections with steroid is not recommended as it may weaken the plantar fascia and lead to rupture. Please refer to “Platelet-rich plasma (PRP) injections” in “Achilles tendonitis” for more details of PRP injections.
Surgical treatment
It may be considered in rare cases with persistent symptoms after 6 months of conservative treatment. Usually around 1-5% of patients with plantar fasciitis require surgical treatment. Surgery can be done to release part of the plantar fascia from the heel bone. It aims at relieving the tension in the painful part of the plantar fascia.
After the surgery, a splint or boot is usually used. The possible complications include infection, injury to the neighbouring blood vessels and nerves, etc. It has been reported that the success rate of surgery is between 70 to 90%. Most patients will be able to bear weight 2 to 3 weeks after surgery. It is essential to continue with proper footwear and stretching exercises, and avoid impact sports to prevent recurrence of symptoms.
References
- Atlas of Human Anatomy. 7th edition. Frank H. Netter M.D. Elsevier.
- Schwartz EN, Su J. Plantar fasciitis: a concise review. Perm J. 2014; 18(1):e105-e107.
- Trojian T, Tucker AK. Plantar Fasciitis. Am Fam Physician. 2019 Jun 15; 99(12):744-750.
- Banik A, Mozaffor SA, Hoque A. Effect of ultrasound therapy on plantar fasciitis. International Journal of Medical Science and Diagnosis Research (IJMSDR). 2019 May; 3 (5): 115-125.
- Ling Y, Wang S. Effects of platelet-rich plasma in the treatment of plantar fasciitis: A meta-analysis of randomized controlled trials. Medicine (Baltimore). 2018; 97(37):e12110.
Written by Dr. Diane Tai Hei-yan
March 2021
